Every 40 minutes, someone in the United States dies from an overdose involving opioids. That number isn't just a statistic; it represents real people who needed help too late. In many of these cases, the person wasn't alone. Friends, family, or bystanders were right there, but they didn't know what to do when the victim stopped breathing. This is why knowing how to use Naloxone Nasal Spray is a critical skill for everyone, regardless of your background. While we can't stop every tragedy, carrying this medication and understanding exactly how to administer it turns a bystander into a lifeline.
The technology has evolved significantly over the last few years. Originally available only with a prescription, the NARCAN Nasal Spray was approved for over-the-counter sales by the FDA in March 2023. This means you no longer need a doctor's permission to buy it at a pharmacy or even online. With naloxone temporarily reversing the effects of opioids by competing at brain receptors, it gives a person fighting for air the chance to breathe again until emergency services arrive. But having the kit isn't enough. You need to know exactly how to use it under pressure.
Understanding the Emergency Landscape
Before you touch the device, you need to understand what you're dealing with. We are currently facing an epidemic driven largely by synthetic opioids like Fentanyl. Unlike heroin or morphine, fentanyl is incredibly potent-sometimes up to 50 times stronger than other opioids. This potency changes the rules of engagement. Research from the Centers for Disease Control and Prevention (CDC) indicates that overdoses involving fentanyl often require multiple doses of naloxone to reverse because the drug stays in the system longer than the initial dose of the rescue medication.
When you see someone struggling, panic can set in immediately. Your heart will race, and your mind might go blank. The key to overcoming this is recognizing the signs early so you aren't reacting blindly. An overdose isn't always dramatic like a movie scene where someone stops moving entirely. Sometimes it's subtle. You might notice someone slumped over on a couch, unresponsive to your voice, or their skin taking on a pale or blue tint around the lips. If you suspect drugs are involved, err on the side of caution.
| Symptom | Normal Intoxication / Sleep | Opioid Overdose (Medical Emergency) |
|---|---|---|
| Breathing Rate | Slow but regular rhythm | Sluggish, shallow, or completely absent (fewer than 8 breaths per minute) |
| Pupils | Dilated (large) or normal size | Pinpoint (very small black dots in the center) |
| Responsiveness | Lethargic but wakes up when shaken | Unresponsive to voice or sternal rub (knuckles on chest) |
| Skin Color | Flushing or normal color | Clammy, cold, pale, or bluish/grey lips and fingernails |
| Noise | Snoring softly | Gurgling or choking sounds (often called 'death rattle') |
The Critical First Steps Before Administration
If you identify the symptoms listed above, time becomes your most valuable resource. Brain damage or death can occur within minutes if oxygen levels drop. There is a specific order of operations that health authorities like the Department of Veterans Affairs and the Mayo Clinic emphasize. Skipping this order can reduce your success rate.
First, call 911 immediately. Do not wait to see if the naloxone works before dialing. Even if the person wakes up, they need professional medical assessment. Ambulance crews are trained to monitor for complications that you might miss. Tell the operator specifically that you have administered or plan to administer naloxone; this helps them prepare for potential withdrawal symptoms once the patient arrives at the hospital.
While waiting for the ambulance, clear the airway. Check inside the mouth for pills or vomiting. Turn the person onto their back and support their neck. Tilt their head back slightly to open the airway. This positioning is crucial for two reasons. It ensures the spray goes directly into the nasal cavity rather than spilling out, and if the person starts to vomit later, gravity can prevent choking. The American Heart Association's guidelines for CPR stress this recovery position if the person regains consciousness but remains unable to protect their own airway.
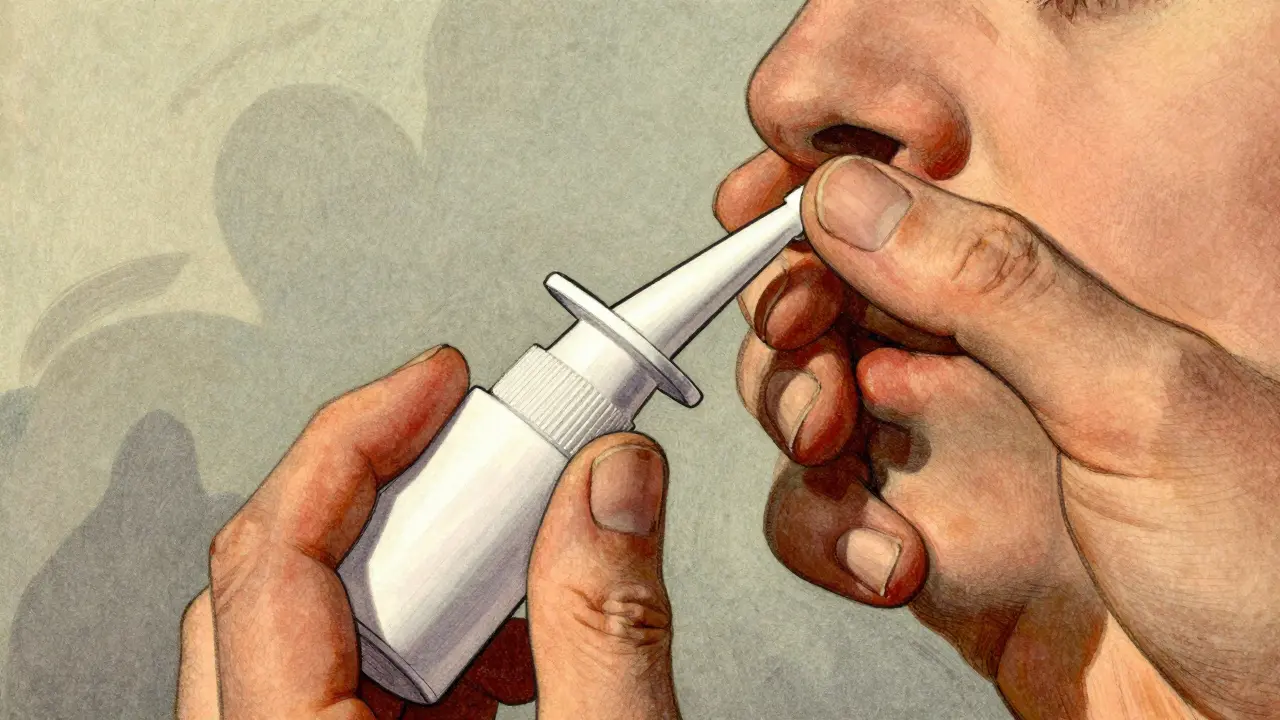
Step-by-Step Administration Protocol
The NARCAN Nasal Spray is designed to be simple, but in a high-stress environment, muscle memory takes over. Follow these steps precisely. Most modern versions deliver a fixed dose of 4 mg of naloxone hydrochloride per spray, though generic or alternative brands may vary slightly.
- Prepare the Device: Remove the package. Hold the device firmly in one hand. The plunger should be ready, but do not push it yet. Some devices have a safety clip that must be removed. Listen for a click indicating the safety mechanism is gone. If you accidentally press it while preparing, the dose is lost, and you must start over with a new unit.
- Insertion: Gently insert the tip of the nozzle into one nostril. Push it in until your fingers holding the base of the nozzle touch the bottom of the nose or the nostril opening. You shouldn't force it deep down; roughly half an inch to an inch is sufficient. According to field studies by the Canadian Centre for Occupational Health and Safety, incomplete insertion is a common error leading to ineffective treatment.
- Deliver the Dose: Press the plunger down fully and steadily. You will feel resistance and then release. Make sure to hold it pressed for a second to ensure the full volume is delivered. Do not tilt the head forward or backward while pressing; keep it level.
- Wait and Monitor: Immediately remove the device. Check for breathing within two to three minutes. Look for a return of chest movement and responsiveness. You can tap their shoulder and shout loudly to test awareness.
- Administer a Second Dose: If the person hasn't started breathing normally after 2-3 minutes, give another dose in the other nostril using a fresh device. Studies show that nearly one-third of fentanyl overdoses require more than one dose to overcome the potency of the synthetic opioids circulating in the blood.
- Monitor for Relapse: If they start breathing, keep them awake if possible. Naloxone wears off faster than some opioids. It has a duration of action of about 30 to 90 minutes. If the person falls back asleep, check their breathing constantly. They can slip back into an overdose state once the medicine leaves their system.
Common pitfalls can undermine even the best intentions. Don't put the nozzle deep into the ear or eye. If you get liquid in their eyes, flush it with water, but do not delay treating the overdose to deal with minor irritation. Another mistake is administering the spray into a blocked nose. If the victim has heavy congestion or bloody discharge in both nostrils, try to clear it gently if time permits, or use the cleaner nostril. Speed matters, but delivery efficacy matters more.
What Happens When Naloxone Works?
You need to know what to expect physically. Naloxone doesn't wake someone up like a shot of espresso. Instead, it knocks the opioids off the receptors in the brain that are suppressing breathing. As the body recognizes the lack of opioids, they enter acute withdrawal. This can feel terrifying for the person waking up. They may vomit, sweat profusely, tremble, or exhibit extreme agitation.
This reaction is actually a sign of success-their breathing has returned, and their body is processing the toxins. Do not restrain the person physically unless they are trying to hurt themselves or you. Trying to force calmness can be dangerous. Keep talking to them calmly until EMS arrives. The withdrawal symptoms are distressing, but they are survivable. More importantly, keeping the patient agitated helps maintain their airway reflexes.
If the person remains unconscious after several doses, you must switch to rescue breathing. If the ambulance is delayed and the victim still isn't breathing after you've done your maximum safe dose of naloxone, you should perform CPR. Focus on gentle breaths into their mouth (rescue breathing) rather than hard chest compressions unless they have no pulse. The Substance Abuse and Mental Health Services Administration (SAMHSA) notes that respiratory support remains the primary intervention; the spray is a tool, not the magic fix-all solution.

Availability, Costs, and Legal Protection
A major barrier to saving lives used to be cost and access. Before 2023, you couldn't buy these easily without a doctor's visit. Now, pharmacies across the US stock the OTC version. Prices vary significantly depending on insurance coverage and location. A standard two-pack usually runs around $140 without insurance, which is expensive for a low-income household, though community health centers and harm reduction organizations often distribute these kits for free or at minimal cost.
Legally, you are protected in 47 states by "Good Samaritan" laws. These statutes explicitly shield anyone acting in good faith during an emergency from liability related to drug possession. So, if you find someone overdosing and call 911 to help, the police generally cannot arrest you or the person for the mere presence of the drugs used in the incident. This policy was designed to encourage people to act without fear of retribution.
Storing the device properly is also part of the job. Keep it at room temperature, ideally between 68°F and 77°F. Avoid leaving it in a car during hot summer days or freezing winter months, as extreme temperatures can degrade the medication. The standard shelf life is 24 months. If the liquid inside looks cloudy or discolored, discard it immediately.
Frequently Asked Questions
Can I use Naloxone on a coma caused by alcohol or benzodiazepines?
No. Naloxone specifically targets opioid receptors. It has zero effect on overdoses caused by benzodiazepines (like Xanax), alcohol, stimulants (cocaine, methamphetamine), or other non-opioid depressants. However, mixed overdoses are very common. If you aren't sure what substance was taken, administer it anyway-it won't hurt the patient.
Is it dangerous to give Naloxone if opioids aren't involved?
It is not dangerous. The medication binds to receptors only if opioids are present. If no opioids are in the system, it essentially does nothing and passes through the body. Medical consensus advises that the risk of an overdose death outweighs any theoretical harm of unnecessary administration.
How many doses of Naloxone do I typically carry?
Most experts recommend carrying at least two kits (4 doses total). One reason is that potent synthetics like carfentanil or fentanyl may require multiple sprays to reverse. Additionally, having a backup ensures you don't run out if the first dose leaks or malfunctions during the attempt.
What is the difference between the 4mg and 8mg sprays?
The 4mg dose (NARCAN) delivers 2mg per nostril and requires spraying in one nostril. The 8mg dose (Kloxxado) delivers 4mg per nostril and is intended for one spray per side. Both are effective, but the 8mg option allows for higher dosage delivery in fewer steps if the patient is known to struggle with severe overdoses or chronic tolerance.
Should I let the person sleep after they wake up?
No. Because naloxone's effect is shorter than the drug causing the overdose, the person can fall back into an overdose state if they fall asleep. Try to keep them awake and sitting up until emergency medical personnel take them to the hospital. If they refuse transport, you must arrange for someone else to stay with them for at least 4 hours.
Carrying naloxone isn't just about following a checklist. It's about being prepared for a moment where someone else's life depends on your ability to think clearly. With practice and knowledge, you become part of the solution in communities affected by addiction and overdose. Whether you are a parent, a teacher, a friend, or a stranger, learning these skills is an investment that pays dividends in human lives.




Kendell Callaway Mooney
March 30 2026This guide breaks down the steps very well for anyone needing quick reference.
I think the part about checking breathing rate is the most important detail to remember.
We often forget to call nine-one-one before trying the spray which is a mistake.
Having the device ready in your glove box or purse is smart preparation.
You never know when a neighbor might slip into a crisis mode unexpectedly.
Please share this with younger friends who might be at higher risk environments.